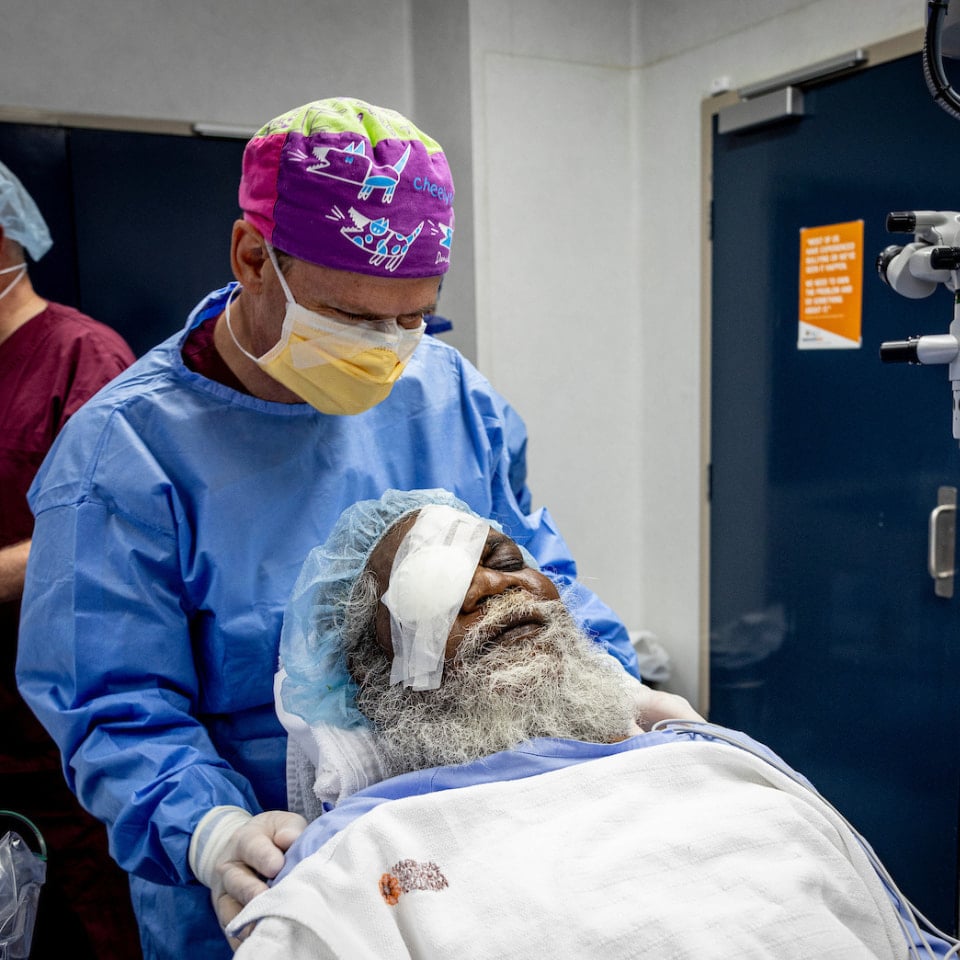
The reality of Indigenous eye health in Australia
Avoidable blindness remains far too common for Aboriginal and Torres Strait Islander people
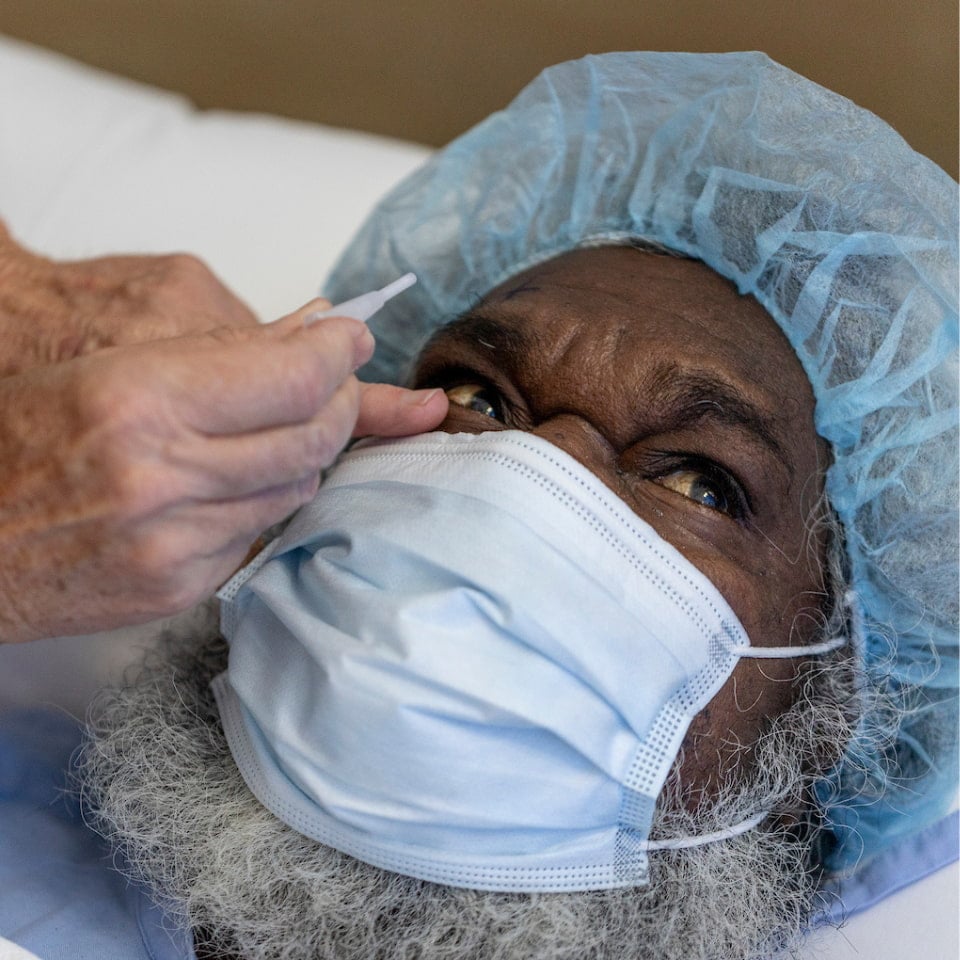
Trachoma still threatens communities
Australia is the only developed country where trachoma still exists, found predominantly in remote Aboriginal communities in the Northern Territory, Western Australia, and South Australia.

Cataracts take sight too soon
Cataract is far more common among Aboriginal and Torres Strait Islander adults, yet people wait almost 40% longer for surgery.
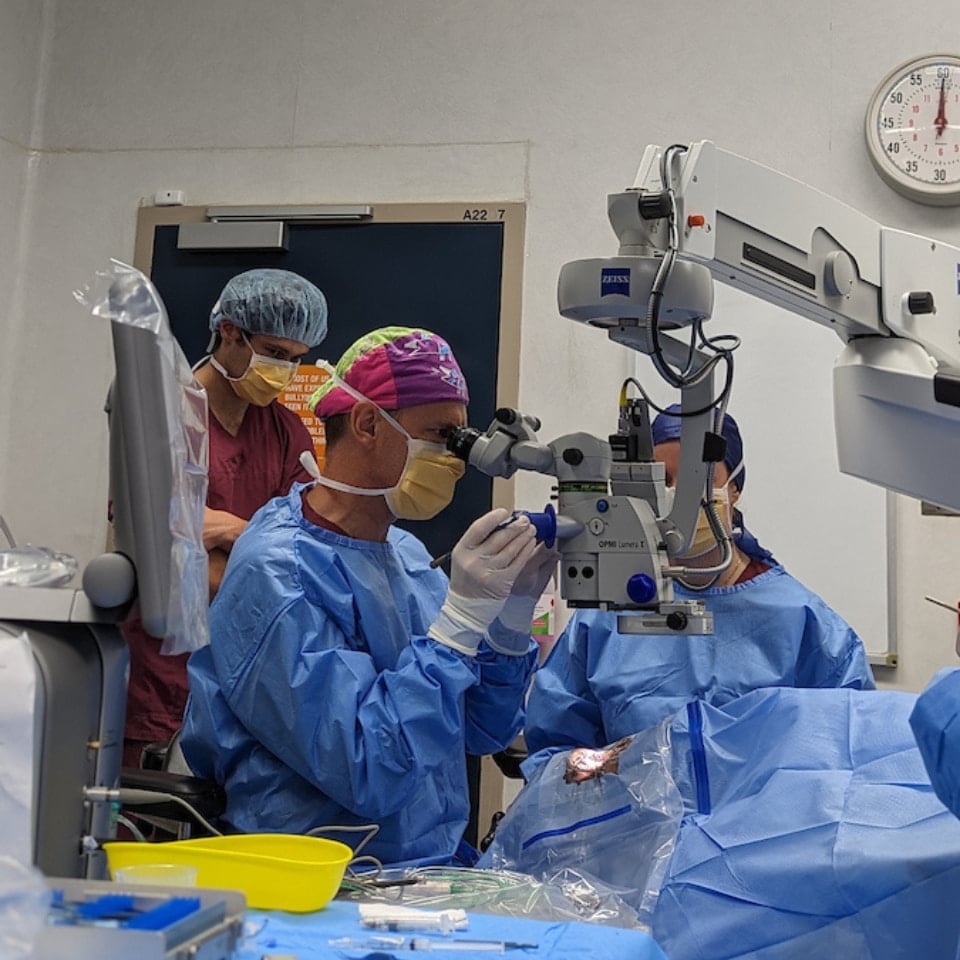
Vision loss limits lives
Blindness and vision loss are three times more common among Aboriginal and Torres Strait Islander adults than among other Australians.
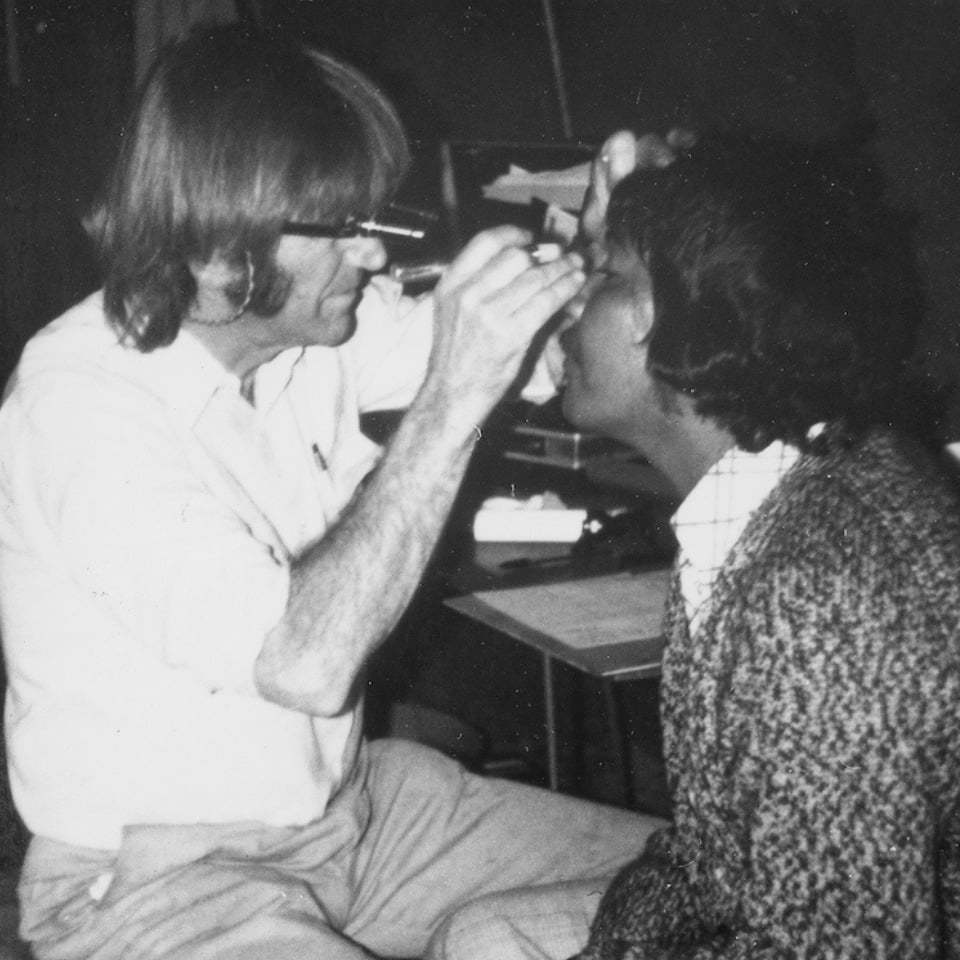
Where our work began: Fred Hollows and Indigenous Australia
In 1968, Fred Hollows was working in his Sydney eye clinic when two Gurindji Elders arrived with eye problems he had never seen before. After treating them, Fred was invited to visit Wattie Creek in the Northern Territory.
He was shocked to find widespread trachoma in remote Aboriginal communities – a disease he believed should not exist in modern Australia.
Fred’s outrage led to the National Trachoma and Eye Health Program. Between 1976 and 1978, Fred and his team visited more than 465 communities, treated over 100,000 people, and halved the rate of blindness among Aboriginal Peoples.
The program’s success came from its approach: First Nations people were involved in the design and delivery of services – a first for health programs in Australia.
As Fred said himself: “Aboriginal groups should be calling the shots, hiring and firing resource personnel, and deciding policy.”
What we’re doing today
Through the Indigenous Australia Program, The Fred Hollows Foundation works in partnership with First Nations–controlled health and community organisations to deliver patient-centred, culturally safe, and community-led eye care.
Thanks to your kindness, in 2024:
- 15,981 people were screened for eye disease
- 3,288 eye operations and treatments were performed
- 3,291 pairs of glasses were distributed
- 78 people were trained, including Aboriginal health workers, educators, and clinic support staff