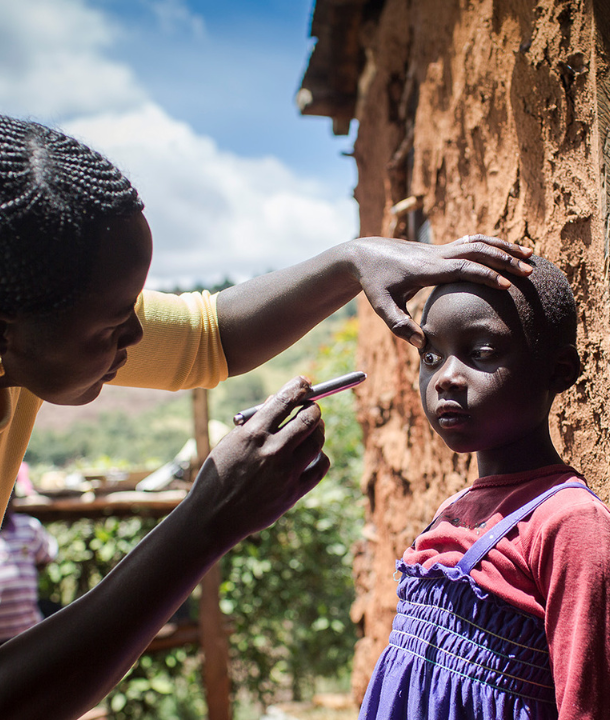
Childhood blindness
Fortunately, vision loss from eye disease in children isn’t very common and most begin life with excellent sight. However, some hereditary, juvenile or inherited diseases can cause visual loss or even blindness early in life. This is a significant problem in developing countries because many families don’t have access to health care and eye health services.
Sadly, the most marginalised people, such as victims of large-scale disasters and displaced people living in makeshift homes, suffer the risk of children dying within a few years of going blind, either from the condition that caused them to go blind or because they live in poverty. But even for the children who do survive with vision loss, life can often be hard if their families aren’t able to look after them properly and access the services they need.
What are the childhood eye diseases we work with?
The common eye diseases that affect children or cause vision loss often depend on the development status of a country. In developing countries, blindness is caused by a number of things: corneal scarring from measles, Vitamin A deficiency, retinopathy of prematurity, trachoma and cataract. The Foundation concentrates on working with our partners to help prevent or treat vision loss in children that suffer from conditions such as:

How can we prevent these diseases?
Early intervention for diseases like cataract and trachoma is critical to correct vision loss in children. But even if the structure and function of the eye are restored to near normal through appropriate glasses or surgery, the capacity to see can’t always be restored. This is because with a child whose brain development has almost been completed (usually by 10 years of age) but who has poor vision, the lack of normal visual stimulation limits the brain’s ability to ever process visual stimuli. To combat the devastating effects of vision loss in children, early detection and appropriate specialist care is essential.
As far as retinopathy of prematurity is concerned, significantly better basic care in local and regional hospitals in developing countries means preterm babies have a good chance of survival. However, many neonatal units are not equipped to screen babies for ROP, so even if they survive, they often have vision loss. We support work in this area through training, and empowering nurses to provide the appropriate oxygen therapy in the incubators and ventilators while the baby is in the ICU. We’re also working to increase awareness within hospitals of the need to have an eye specialist examine and treat babies even while they are in the ICU.
Disclaimer: the content on this page is not intended to be medical advice. For medical advice, please contact your local health professional.

