Diabetic retinopathy: what it is, why it matters, and how to protect your sight

Have you heard of diabetic retinopathy?
Diabetic retinopathy is an eye condition caused by diabetes. It can damage the retina (the light‑sensitive layer at the back of the eye) and, without treatment, can lead to vision loss.
It is one of the leading causes of avoidable vision loss in working‑age adults worldwide. As more people are living with diabetes, protecting eye health is becoming even more important.
Below, we explain what diabetic retinopathy is, the signs to look out for, how it is diagnosed and treated, and the simple steps you can take to reduce your risk. We also share how The Fred Hollows Foundation works with partners to strengthen screening and treatment pathways around the world and eliminate all forms of avoidable blindness.
Key takeaways: Diabetic retinopathy often has no symptoms early on. If you have diabetes, regular retinal screening can find problems early,when treatment is most effective.
For more information, visit the diabetic retinopathy page of our website.
What is diabetic retinopathy?
Diabetic retinopathy happens when longstanding and/or uncontrolled diabetes damages the small blood vessels in the retina. It usually develops slowly, and many people don’t notice any changes in their vision at first.
If diabetic retinopathy is not found and treated in time, it can cause permanent vision loss. The good news is that regular screening and timely treatment can prevent most severe vision loss from diabetic retinopathy.
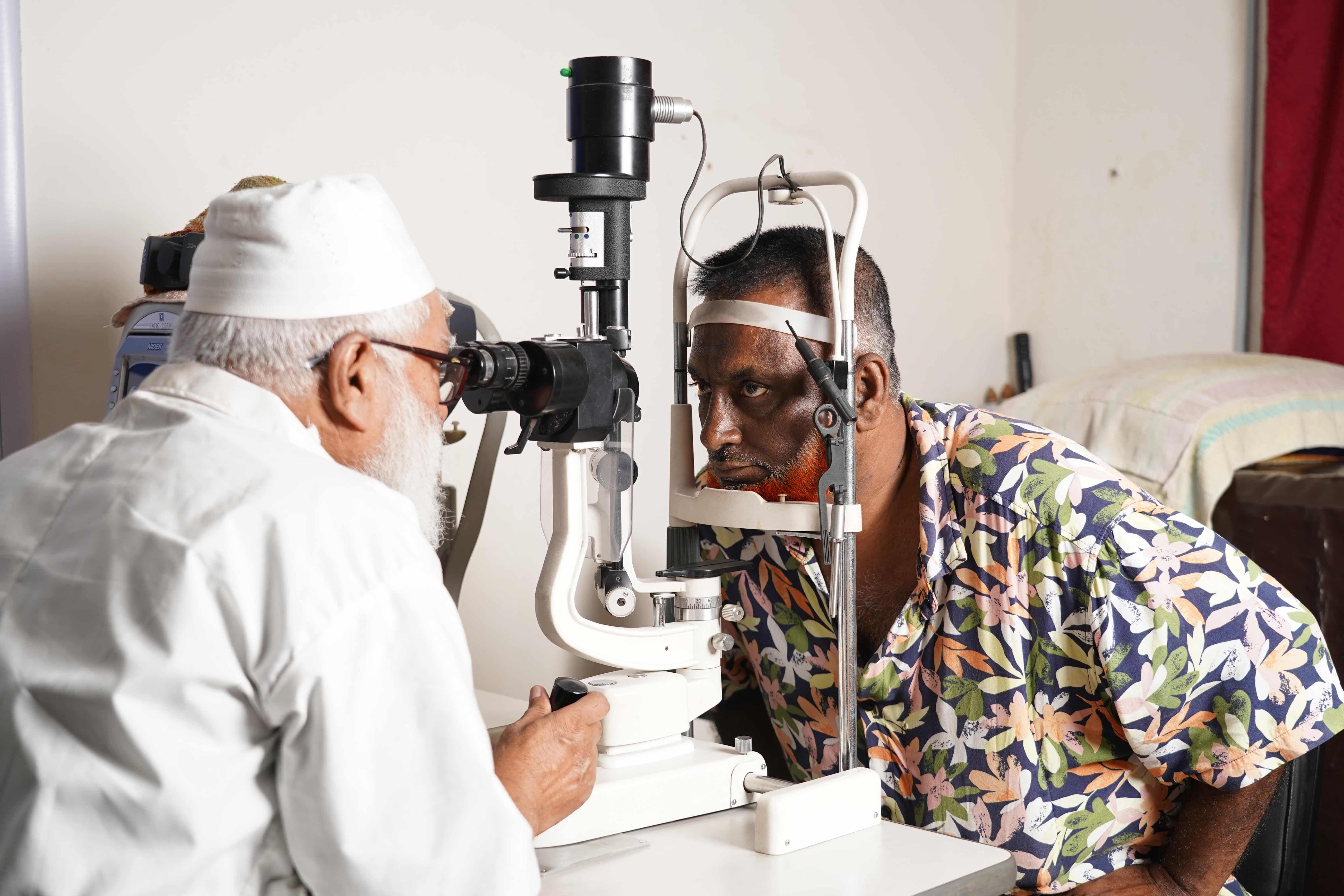
After years of vision loss caused by diabetic retinopathy, Nazmul Hossain can see again following sight-saving treatment in Barisal, Bangladesh.
Photo credit: Rubel Karmaker
How is it caused?
Diabetic retinopathy can affect people with both type 1 and type 2 diabetes.
Over time, high blood sugar can damage the tiny blood vessels in the retina. High blood pressure and high cholesterol can also increase risk. The longer someone has diabetes, the greater their risk of developing diabetic retinopathy.
How can you avoid it?
The challenge of this condition is that, in its early stages, there are often no symptoms and hence many people don’t know they have diabetic retinopathy until it becomes more serious. Early detection through regular retinal screening and timely treatment are the most significant ways to reduce the risk of severe vision loss.
That’s why regular retinal screening and health check ups is essential for maintaining good eye health in person having diabetes
How is diabetic retinopathy diagnosed?
When you go for a comprehensive eye examination, your ophthalmologist will use a number of strategies to determine if you have had any imperceptible changes to your eye health or sight.
Dilated Eye Exam
This often includes the use of eye drops that widen the pupils. This allows your retina to be seen more clearly and any leaking blood vessels, swollen vessels or new vessel growth to be more readily identifiable.
Retinal Photography
Using modern technology, special imagery can be taken of the back of your eye. This record can be compared with previous pictures and used to check what changes, if any, have occurred.
Optical Coherence Tomography
Optical Coherence Tomography (or OCT for short) is a completely pain-free scan that produces a cross-section image (or images) of your eye. It helps doctors determine if there is any worrying swelling.
How often should you get an eye health check or screening?
Organised eye health screening in a clinic, community health centre or even via telehealth services helps detect diabetic retinopathy as early as possible.
For underserved communities with limited access to health care and who are at greater risks, this can be vision-saving.
Many people with diabetic retinopathy experience no symptoms until the far more advanced stages.
We recommend regular retinal screening if you have been diagnosed with diabetes, at least once a year. However, your eye health professional may suggest more regular check-ups if needed or associated with risk factors like high blood pressure, high cholesterol etc. If you have not been diagnosed with diabetes, a screening every one or two years is best practice.
How is The Fred Hollows Foundation helping to deliver DR screenings around the world?
The Fred Hollows Foundation works with local partners and governments to strengthen diabetic eye care, especially in places where people face barriers to getting the services they need to ensure they have access to much-needed eye health screening and treatment.
- Building a full pathway from screening to treatment—because screening only helps if people can get the follow‑up care they need.
- Integrating retinal screening into diabetes and noncommunicable disease (NCD) services, so care is closer to where people live.
- Training and supporting local health workers, and strengthening referral and follow‑up systems so patients are not lost between services.
- Providing equipment and technical support, such as retinal cameras and, where appropriate, using telehealth and AI‑assisted workflows to help services reach more people.
- Supporting quality and data systems to track screening, referral and treatment, so services can improve over time and reach the people most at risk.

Mary from Siaya County lost her sight to diabetic retinopathy, forcing her to rely on family and give up her work. After free screening and surgery, her sight has been restored, and she is back farming and supporting her community.
Photo credit: Mary Odhiambo
What are the main stages of diabetic retinopathy?
Diabetic retinopathy usually progresses through a few stages. The more advanced the stage the greater the risk to your vision.
These stages include:
1. Mild non‑proliferative diabetic retinopathy
During this stage, small bulges (microaneurysms) occur in your retinal blood vessels. In most cases, there are no obvious symptoms at this stage.
2. Moderate to severe non‑proliferative diabetic retinopathy
As more and more vessels become blocked or begin to leak, there is an increased risk of swelling in the central retina, known as the macula, which can affect sharp, detailed vision.
3. Proliferative diabetic retinopathy
At this stage, new and fragile blood vessels begin to grow on either the retina and/or the optic nerve, Over time this can cause bleeding and scar tissue formation and, in more severe cases, retinal detachment.
4. Diabetic macular oedema (DMO)
DMO occurs when fluid leaks into the macula. Being the part of the retina that is responsible for providing sharp and central vision, this stage of diabetic retinopathy can cause blurred and distorted vision
What happens if it is left untreated?
When untreated, diabetic retinopathy can develop and worsen causing permanent and sometimes quite rapid loss of vision.
This occurs when there is:
- Progressive damage to the retinal blood vessels, leading to more bleeding and leakage.
- Scar tissue formation, which can pull the retina away from the back of the eye.
As mentioned at the top, diabetic retinopathy is one of the leading causes of preventable blindness in many countries.
What are the main symptoms of diabetic retinopathy?
As mentioned, symptoms do not always show up during the early stages of this condition. However, possible symptoms to watch out for include:
- Blurred vision
- Fluctuating vision
- Dark spots, floaters or cobweb‑like shapes in your vision
- Difficulty seeing at night
- Difficulty reading fine print
- Dark or empty areas in your field of vision
- Sudden vision loss
Seek urgent help if you have sudden vision loss, a sudden increase in floaters, flashes of light, or a dark “curtain” in your vision. These can be signs of serious eye problems that need immediate assessment.
How is diabetic retinopathy treated?
The right treatment will depend on the stage and level of severity of the disease. There are a number of options however to help prevent or reduce the risk of vision loss.
- Laser therapy (photocoagulation)
- Anti‑vascular endothelial growth factor (VEGF) injections
- Steroid injections or implants
- Vitrectomy surgery
- Systemic risk factor control
How can you reduce your risk of diabetic retinopathy?
- Ensure you get regular eye checks
- Keep your blood sugar, blood pressure and cholesterol monitored and controlled
- Take diabetes medicines if necessary
- Avoid smoking
- Maintain a healthy weight
- Lead an active lifestyle
- Seek medical care promptly if you notice any change to your vision
Frequently Asked Questions About Diabetic Retinopathy
How often should I get an eye health screening if I have diabetes?
It is recommended that you get an eye check when you are first diagnosed with diabetes and then at least once a year from that point, unless advised otherwise by a qualified medical professional.
Is it possible to have diabetic retinopathy if I have good vision?
Unfortunately, yes. Symptoms can take a while to develop when it comes to diabetic retinopathy.
Is diabetic retinopathy painful?
Not usually. However, whilst there is not often pain, there can be disruptive and concerning changes to your vision.
Will my vision improve if I get my blood sugar under control?
Maintaining good blood sugar control will slow progression and reduce the risk of additional damage, but it cannot reverse or reduce damage already incurred. We recommend seeing your eye health specialist to ascertain the right treatment for your needs.
How can remote or low-income‑ communities access screening and treatment?
The Fred Hollows Foundation is working hard and using new technologies such as portable retinal cameras, telehealth and AI supported‑ screening, alongside our training programs, referral systems and patient follow‑up, to widen access and improve service for under‑served regions throughout the world so that early screening and diagnosis leads to timely care.
How can you support The Fred Hollows Foundation?
Our mission at The Fred Hollows Foundation is to end avoidable blindness. Our team does this by preventing and treating eye diseases, such as diabetic retinopathy by supporting eye health services in Australia and around the world.
We train local eye health workers, equip local clinics with essential equipment to enable them to provide eye checks and timely treatment to their communities.
There are many ways to help end avoidable blindness. Find out how you can get involved or connect with our team to learn more about supporting this work.
Meet the author
Learn more about eye health
Your eyes as health monitors: what eye exams reveal about overall wellness

The hidden cost of poor vision: why ending avoidable blindness matters to all of us